Key Messages
Women can feel pain differently during labour. Some women cope with labour and birth without pain medication and other women want or need pain medication.
During labour, the muscles in your uterus will alternately contract and relax. You will feel your abdomen become hard to the touch and then relax with each contraction. Contractions occur during labour to help your cervix open up and to help push your baby out. This is painful for most women.
Some women plan to go through labour without pain medication and others plan to use pain medication. Sometimes women change their minds about pain medication use during labour. It is helpful to keep an open mind about how you will manage your pain in labour. Inform yourself about the risks and benefits of medical pain relief before labour begins. It is also helpful for you to know, ahead of time, the pain control options available at your place of birth.
You may find it more difficult to cope with labour if:
- You lack confidence and are not prepared for labour and birth.
- You feel overly fearful or anxious about the process of labour and birth.
- You are not well-rested.
- You do not have a support person to be with you during labour and birth.
- You are not able to change your position or move around during labour.
- Your baby is in a position that gives you more back pain.
- Your labour has been induced or is longer than expected or you have had other medical interventions.
- You have a low tolerance for pain.
- You have experienced a traumatic experience in your past.
There are different pain medications to help women cope with labour pain. Options available to you depend on where you give birth and your stage of labour.
Pain medications come in a variety of forms. Some relieve pain more than others and some relieve pain for a longer period of time. You may not know which type of pain control will work best for you until you are in labour. Talk to your health care provider about the pain control options you may want to try during labour. When in labour, choose the method(s) that works best for you and your baby.
Pain medications used in labour can be divided into several categories:
- Non-opioid analgesics, which can provide mild-to-moderate pain relief. They are usually taken orally.
- Opioid analgesics, which can provide moderate-to-strong pain relief. They can be given by injection or intravenously.
- Anesthetics, which can provide a range of pain relief including almost complete pain relief. Nitrous oxide (i.e., laughing gas), epidurals, and pudendal nerve blocks are examples of anesthetics.
For information about transcutaneous nerve stimulation (TENS), acupuncture, and other ways of coping with the pain of labour, please see the Labour Support file.
Pain medications have risks as well as benefits for you and your baby.
Some pain medication may have side effects. Learn about the side effects of any medication you are considering. Some side effects might include:
- Nausea and/or vomiting.
- Dizziness and/or weakness.
- Decreased ability to walk and/or change positions.
- Itchiness.
- Headaches.
- Concerns for the baby during labour or at birth.
- Increased risk of assisted vaginal birth.
Note that these side effects do not apply to all medications.
If you are close to giving birth, the type of pain medication you can safely have may change.
If certain pain medications such as narcotics are given too close to birth, they can cause your baby to have breathing difficulties at birth. They will not be used if your baby’s birth is expected within two to four hours. Your health care provider will do a vaginal exam before you receive pain medication to make sure that you are not too close to giving birth. If you are very close to giving birth, you can still receive pain medication but the type or amount of the pain medication may change.
You and your baby will be monitored more closely if you use pain medication in labour.
How often your blood pressure, heart rate and breathing rate is checked will depend on the medication used. In some cases, your baby’s heart rate will need to be monitored continuously for a period of time.
If you or your baby experience side effects from the medication, your health care provider can try to reduce these side effects by:
- Reducing or removing the medication.
- Changing your position.
- Giving you intravenous (IV) or oral fluids.
- Giving you, or your baby, other medication to counteract the effects of the pain medication.
- Giving you oxygen (in some instances).
Learn more about pain medications in labour
You can find out more about pain medications in labour from the following resources. More suggestions can be found in the Resources and Links section.
- Your health care provider
- Canadian Anesthesiologists’ Society (CAS)
Supporting Evidence
About Medical Pain Management
Labour pain
During labour, most women experience pain.1,2,3 Pain is a normal and expected part of labour.4,5 In the first stage of labour, a woman’s uterine muscles contract and her cervix dilates. Uterine contractions are typically painful. The pain experienced with contractions can also radiate to a woman’s back, buttocks, and thighs.
Between contractions, a woman’s uterus rests and she usually feels no associated pain. Contractions can feel cramp-like at first but as a woman’s labour progresses and her cervix dilates further, they tend to become stronger, more frequent, and last longer. A typical contraction in active labour occurs about five times in 10 minutes and lasts 50 – 60 seconds.
Typically, the most painful and most frequent uterine contractions occur at the end of the first stage of labour as a woman’s cervix reaches full dilation. Once she has reached full dilation, she may not have an urge to push right away. Once she feels the urge to push, the pain experienced is a combination of uterine contraction pain and pain associated with distension of the vagina, perineum, and the pelvic floor as the baby is pushed through the birth canal.1,2,3
A unique experience for each woman
Although pain is a normal and expected part of labour, women experience pain differently during labour.1,3,6 Some women report feeling minimal pain during labour and some women report that it was the most severe pain that they experienced in their lifetime.1
The degree of pain and each woman’s ability to cope with it can depend on a number of different factors. These factors can be both physical and psychological in origin, including:1,6,7,8,9,10,11
- A woman’s parity. Nulliparous women may experience a greater sensation of pain than multiparous women especially before 5 cm dilatation.9
- A woman’s prior experience(s) with labour.
- A woman’s prior experience(s) with pain.
- A woman’s degree of preparation for labour.
- A woman’s confidence in her ability to give birth and cope with labour pain.
- The support that a woman receives during labour.
- The environment during labour.
- A woman’s cultural beliefs about pain and childbirth.
- The position(s) a woman assumes during labour.
- A woman’s ability to move around and change positions during labour.
- The position of the fetus.
- How the labour is initiated (spontaneous or by induction).
- The quality and strength of a woman’s uterine contractions.
- The need for medical interventions such as assisted vaginal birth.
Options to relieve labour pain
Several options are available to help women cope with labour pain. Some women use non-pharmacological measures (i.e., no pain medication during labour) and other women use pharmacological measures (i.e., administration of one or more types of pain medication during labour).
Non-pharmacological measures can be preferred or may be relied upon for as long as possible during labour as pharmacological pain relief methods may present risks for a woman and her fetus.1,2,4,7,12,13,14 Women need to know they will be supported no matter how they choose to manage their labour pain.
Pharmacological measures may be considered at any point during labour and may help reduce the potential for:1,6,15,16
- Hyperventilation and a reduction in the supply of oxygen to the mother and fetus.
- A prolonged labour.
- Difficulty in pushing effectively.
- Long-term emotional and psychological ramifications.
Women should be informed of the benefits, risks, and alternative pain-management options in labour and should choose the method best suited to them.1,5,7,13,17
Women are encouraged to speak with their health care provider prior to their labour to discuss the options available to them for pain relief in labour in their chosen birth setting.14,18
The use of pain medication is growing among women in labour, especially the use of epidurals.19,20
Nitrous oxide
In 2007, 78 percent of hospitals in Canada and 83 percent of hospitals in Ontario had nitrous oxide available for pain relief during labour. In 1993 in Canada, only 68 percent of hospitals had nitrous oxide available for pain relief during labour. About one in five Ontario women (19 percent) used nitrous oxide for pain relief during labour.21 In a survey of women in 2006 in Canada, nitrous oxide had one of the lowest ratings for being “very helpful” for pain relief during labour.19
Narcotics
In 2007 in Canada, 98 percent of hospitals had narcotics available for pain relief during labour. This number increased slightly from 94 percent in 1993. In 2006 in Canada, 33 percent of women used narcotics for pain relief during labour.21
Epidurals
The largest increase of a pharmacological method for pain relief during labour has been the use of epidurals.20, 22 In 1993, only 55 percent of hospitals in Canada had epidurals available for pain relief during labour; in 2007 in Canada, this had increased to 87 percent of hospitals having epidurals.21 In 2011 – 2012 in Ontario, it was reported that 63.1 percent of women who had a live vaginal birth used an epidural or spinal-epidural combination for pain relief during labour; this was increased from 61.1 percent in 2007-2008.20 Furthermore, in 2006, 81.1 percent of women who had an epidural or spinal anesthesia believed that it was “very helpful” for pain relief.19
In 2006, hospitals were asked if epidural anesthesia was available 24 hours a day and 79 percent of hospitals indicated that was the case. Large hospitals and university teaching hospitals were more likely to have epidural anesthesia available 24 hours a day.21
Options for Pain Medication during Labour
Pain medication can be described as either an analgesic or an anesthetic.
Analgesic medication typically results in the reduction of the sensation of pain. It does this by binding to and blocking different pain receptors in the body. It does not result in the loss of feeling of a body part or the loss of consciousness. Analgesic medication can be classified as either an opioid or a non-opioid. Non-opioid medications tend to only provide women in labour with mild-to-moderate pain relief, but since they do not present many risks for a woman or her fetus, they can be a preferred option.10,14,23 Opioid medications chemically resemble morphine. Opioid medications fall into the broad class of medications referred to as narcotics, a powerful class of analgesics that have varying degrees of potency and duration. Narcotics cannot be bought over-the-counter as they are controlled substances. Narcotics typically provide some pain relief for a woman in labour but are associated with a variety of risks for a woman and her fetus.1,3,6,24
Anesthetic medication acts as a pain medication as it results in the temporary loss of feeling of a body part or the loss of consciousness. It does this by blocking nerve impulses being sent to the brain in an area of the body. Its effect depends on the type of anesthetic medication, the dose, and how it is given.6,14 See the sections on anesthetics for more information on anesthetic medication use in labour.
A woman may choose to have a different classification of pain medication during different stages of her labour depending on her needs. Women should be aware of the benefits, risks, and limitations of pain medications before labour begins.7,17
Non-opioid Analgesics
Non-opioid pain medications only provide mild-to-moderate pain relief, but they are still beneficial in providing pain relief especially during early labour.10,23 Non-opioid medications involve a pharmacological mechanism referred to as a ‘ceiling effect.’ The ceiling effect means that once an upper limit or ceiling has been reached, taking more of the medication will not provide any further pain relief. A health care provider may choose to give non-opioid analgesics with other medications that potentiate their effect.10,25
Most non-opioids are considered safe when used for temporary, acute pain. Problems usually arise when people take them over a longer period of time. Chronic use of non-opioid medications can result in damage to a person’s gastrointestinal tract, kidneys, liver, and other organs. Non-opioid medications considered safe for pain relief during labour involve acetaminophen and some sedatives.1,10,14,23
Most non-opioid medications are available over-the-counter without a prescription and are taken orally. Women should be encouraged to discuss the use of non-opioid medications during labour with their health care provider.
Acetaminophen
Acetaminophen is commonly referred to by its trade name Tylenol. It works to relieve mild-to-moderate pain but only for a short period of time. TYLENOL and TYLENOL Extra Strength may be suggested for discomforts of early labour.10,23
Opioid Analgesics
Opioid analgesics, or narcotics, are a class of analgesics which includes many different drugs with varying degrees of potency, times of onset, durations of action, and side effects. They are typically used to treat moderate-to-severe pain.
Narcotics, which are commonly used for pain relief during labour, include morphine; hydromorphone (Dilaudid); fentanyl (Sublimaze); sufentanil citrate (Sufenta); nalbuphine hydrochloride (Nubain); and others. The narcotic used depends on the birth setting as well as the stage of labour.1,7,10,14,24
Women should be aware of the risks associated with using narcotics for pain relief in labour. These risks include:1,2,3,7,10,14,15,26
- Nausea.
- Vomiting.
- Dry mouth.
- Constipation.
- Urinary retention.
- Itchiness.
- Dizziness/weakness.
- Sleepiness/drowsiness.
- Hallucinations.
- Decreased ability to safely ambulate independently.
- Low blood pressure.
- Fast or slow heart rate.
- Maternal respiratory depression.
- Decreased fetal heart rate and/or decreased fetal heart-rate variability.
- Fetal or neonatal sedation and/or respiratory depression as narcotics readily cross through the placenta and take time to be eliminated from circulation.
- Incomplete pain relief.
- Delayed breastfeeding initiation.
Narcotics can be administered via an intramuscular (IM) injection or an intravenous (IV) infusion. The route is often determined by the type of narcotic as well as the stage of labour.1,3,7,14
Intramuscular injections
During labour, a woman can receive narcotics for pain relief via an injection given in her upper arm muscle, upper thigh muscle, or gluteal muscle. This is called an intramuscular injection.14 Morphine, hydromorphone (Dilaudid), and nalbuphine hydrochloride (Nubain) are common narcotics given for pain relief during labour via an IM injection.
Advantages of receiving pain medication via an IM injection include:14
- Quick administration.
- No need for an IV line.
Disadvantages of receiving pain medication via an IM injection include:3,7,14
- Sometimes a delayed onset of pain relief.
- The need for high doses of medication.
- An unpredictable rate of release of medication from muscle tissue that can result in uneven distribution of the medication.
- The inability to give medication close to birth with this method as there may not be enough time for it to be eliminated from fetal circulation prior to birth.
Intravenous infusion
During labour, a woman can receive narcotics for pain relief via an IV infusion. To administer a pain medication via an IV, the IV is stopped, and the medication is given slowly in an IV port. Fentanyl (Sublimaze) and sufentanil citrate (Sufenta) are common narcotics given via an IV for pain relief during labour. When fentanyl or sufentanil is given via IV, it typically begins to work within two to five minutes, peaks within three to five minutes, and lasts for 30 to 60 minutes. Sufentanil use is increasing because it has more potent effect and does not affect the baby as much as other narcotics.14
Intravenous patient-controlled analgesia (PCA) is available in some hospitals. For this, an IV pump is programmed to allow a woman to push a button to self-administer a small dose of a narcotic such as fentanyl when she needs it in labour. Most of the time, there is also a base infusion rate and the woman tops this up as needed. An IV PCA allows for more maternal control of pain control during labour. It is also sometimes reserved for women not eligible for an epidural.24,27
Advantages of receiving pain medication via an IV, as compared to an IM injection, include:14
- A quicker onset of action.
- The need for smaller doses of medication.
- A more predictable effect.
Disadvantages of receiving pain medication via an IV, as compared to an IM injection, include:14
- The need for more frequent administration of the medication.
- Restricted movement due to the IV set-up.
Please note that all narcotics cross the placenta, so there is an increased need to assess the baby at birth.7,14,24,27
Anesthetics
Nitrous oxide is a medication used by women for pain relief during labour. It is a blend of 50 percent nitrous oxide and 50 percent oxygen. To use the medication, a woman inhales the gas through a mouthpiece or facemask attached to either a single, portable premixed cylinder called Entonox or through a small, regulatory apparatus called Nitronox attached to either two portable cylinders or a hospital pipeline.2,7,18,28
Advantages of using nitrous oxide for pain relief during labour include:15,18,28,29
- It is non-invasive.
- It is self-administered by the woman.
- It is fairly easy to use.
- It can be used at a variety of times during labour (e.g., while waiting for other pain medication to be prepared or during the transition period when pain can become intense).
- It provides physiological pain relief as well as psychological distraction from contraction pain.
- It has no odour.
- It is eliminated fairly quickly from a woman’s body.
- It crosses the placenta, but it is eliminated fairly quickly from fetal circulation in comparison to narcotics.
Nitrous oxide is believed to suppress pain stimuli transmitted to the brain.1,30
To use nitrous oxide during labour a woman is instructed to:2,14,18,28
- Insert a mouthpiece or cover her mouth and nose with a facemask and breathe in the gas as a contraction begins. It takes 50 to 60 seconds for the gas to start to work which is why a woman is encouraged to begin to breathe in as soon as a contraction begins.
- Inhale slowly and deeply until the contraction subsides for best pain relief. The gas is only released when a woman inhales as this opens a valve. When a woman stops inhaling, the valve closes.
- Exhale into the mask to reduce exposure to others in the room.
- Remove the mouthpiece or facemask between contractions and breathe normally.
Nitrous oxide can provide good pain relief, but it does not eliminate all pain. Some women like it and find it is helpful to them during labour.14,15
Adverse effects of using nitrous oxide during labour include:1,2,7,14,15,18,28
- Nausea.
- Vomiting.
- Dizziness.
- Drowsiness.
- Hallucinations.
- Hyperventilation or hypoventilation.
- Maternal and fetal hypoxia.
- Loss of consciousness (extremely rarely and usually only if narcotics are also being used).
The risk of some of these adverse effects can be minimized if a woman takes breaks from inhaling the gas and breathes normal air deeply. To avoid adverse effects, the woman should also be the only one to hold the mouthpiece or the facemask to her face to administer the medication.15
An epidural involves the insertion of a needle between two vertebrae in a woman’s lower back to deliver medication into her epidural space (i.e., the space surrounding her spinal column). Only an anesthesiologist or other health care provider specifically trained in this technique may perform an epidural.6,31,32 The pain medication used for an epidural can consist of a narcotic (i.e., fentanyl or sufentanil), an anesthetic medication (i.e., bupivacaine or ropivacaine), or both. Depending on the type and the amount of the medication used, a woman can experience partial or complete pain relief and varying degrees of motor impairment.6,14,31
Benefits of receiving an epidural during labour include the following.6,7,14,15,33
- It is the most effective pain relief medication for women in labour.
- The fetus is at less risk of side effects as compared to systemic narcotics which can cause neonatal respiratory depression.
Risks associated with receiving an epidural during labour include:1, 6,7,14,31,32,33,34
- Decreased ability to move around and change positions during labour due to a potential motor block and the IV line needed with an epidural.
- Lower back pain from the insertion of an epidural needle. Sometimes multiple attempts are needed to find the epidural space.
- Dizziness and/or weakness.
- Difficulty voiding and the need for catheterization.
- The inability to feel the urge to push.
- Prolonged labour.
- Assisted vaginal birth.
- Ineffective pain relief.
- Itchiness.
- Fever.
- A tingling sensation in the lower limbs called paresthesia.
- Hypotension. A 20 percent drop in blood pressure or a blood pressure of less than 100 mm Hg systolic can result in maternal and fetal oxygen deprivation.
- Postdural puncture headache.
- Delayed breastfeeding initiation and possible early breastfeeding cessation.
- Extremely rarely, infection.
- Extremely rarely, maternal respiratory depression.
- Extremely rarely, maternal neurological-related problems or respiratory arrest.
IV fluids and medications can be given to counteract side effects such as a drop in maternal blood pressure, nausea, or itching.14 See the section on coping with adverse reactions for more information.
Contraindications
Some women are not eligible to receive an epidural during labour.
Epidural may be contraindicated if a woman:14,31
- Has a bleeding disorder and/or is taking anticoagulants. For these women, injury to a blood vessel can cause a hematoma to form that can compress the spinal cord and lead to serious neurological complications.
- Has an infection in the area of her lower back which is at risk of spreading if punctured.
- Has experienced a back injury or has a back-related medical condition such as scoliosis.
For a woman with a lower-back tattoo, direct puncture of it should be avoided if possible as the epidural may not be effective if the tattoo is punctured. There is, otherwise, no evidence-based reason to deny an epidural for a woman with a lower-back tattoo.35
Women who have concerns about whether they are a candidate for an epidural can request an anesthesia consult during the prenatal period.
Epidural initiation
The process of receiving an epidural involves many steps. This process often occurs when a woman is feeling moderate-to-severe pain. Thus, it can be helpful to a woman and her support person to review the process in advance if a woman is anticipating receiving an epidural during labour.
To receive an epidural, the process is as follows:6,7,14,31,32
- Informed consent is obtained from the woman by the health care provider doing the procedure.
- The fetal heart rate is checked prior to the initiation of an epidural to ensure that it is normal.
- An IV line is initiated. A normal saline solution or Lactated Ringer’s solution is infused through the IV. A woman may receive a bolus dose of 500 mL – 1000 mL of fluid prior to the epidural to prevent hypotension, but such pre-loading is not always done.
- Those in the room are sometimes asked to wear a mask and stay in front of the woman as the process is a sterile procedure. To avoid overcrowding, usually only one support person is permitted in the room.
- The woman is asked to sit or lie on her side with her back curved to allow the space between her vertebrae to widen.
- The physician applies antiseptic solution to the woman’s back and then applies pressure with a finger to the woman’s lower back to determine where the epidural needle will be inserted.
- The physician uses a fine needle to administer a local anesthetic to numb the area. It can feel like several tiny pinpricks when this is done. The area is numbed so that a woman does not feel the insertion of the larger epidural needle.
- A nurse, midwife, or support person may face the woman and place his or her hands on her shoulders to help her to remain still during the placement of the epidural needle. It is important to remain still during the insertion to prevent misplacement.
- The physician inserts the epidural needle between contractions. A woman typically feels pressure when this done. The insertion may need to be done more than once to find the correct space.
- Once the space is identified, 3 cm – 5 cm of a very fine plastic epidural catheter is inserted into the epidural space and the needle is removed. Pain medication is given through this catheter.
- A test dose may be given to ensure that the catheter is in the correct space. This involves the administration of epinephrine through the catheter. If a woman’s heart rate increases following the dose, this may indicate the health care provider is in a blood vessel. This test is not always accurate, and thus it may not be done.
- The catheter is taped to the skin of the woman’s back, so it does not move.
- Intermittent, continuous, or patient-controlled epidural with an analgesic medication, anesthetic medication, or both is initiated. The method and type of medication used often depend on its availability at the institution and/or the needs of the woman in labour.
Following the initiation of an epidural, a woman will typically be positioned with the head of her bed slightly elevated. Her blood pressure, heart rate, respiration rate, and oxygen saturation will be checked every 5 to 10 minutes for 30 minutes and regularly thereafter to ensure maternal well-being.
The level of a woman’s loss of feeling (or sensory block), as well as her ability to move her legs (or motor block), will also be assessed. Sometimes ice is used to assess the sensory block. Where there is no block, the ice will feel colder compared to where there is a sensory block. If a woman is wedged to one side, to ensure that symmetrical sensory and motor blocks are achieved, a woman should try to rotate from side to side. If a sensory block is too high (i.e., above the nipple line, which can impede the act of breathing), a health care provider may raise the head of the bed.2,14,31 See the section on coping with adverse reactions for more information.
Following the initiation of an epidural, the fetal heart rate will also be regularly checked. Continuous fetal heart-rate monitoring is not required unless there is concern about the fetus.36
If maternal and fetal vital signs are normal, a woman with an epidural can be encouraged to move and change positions. This can be good for her circulation as well as to help her fetus descend into her birth canal.37 If the epidural and hospital policy permits the woman to walk, she should always undergo a supervised step-test first. This involves the woman first sitting on the side of her bed. If while sitting she does not feel dizzy or lightheaded, she can try to stand. If she still does not feel dizzy or lightheaded, she can try to take to take three unassisted steps with accompaniment. Even if a woman is able to walk with an epidural, she should still be accompanied by one or more persons while walking to prevent injury from falling in the case of weakness.14
Intermittent, continuous, or patient-controlled epidural
With an epidural, pain medication is always delivered as a solution through the epidural catheter in a woman’s lower back, but the method of administration can vary. The method used can depend on the availability at the hospital as well as a woman’s needs during labour.2,6,14,31
Intermittent method
With this method, a health care provider trained in anesthesiology directly injects the pain medication into the epidural catheter when a woman requires pain relief. For sufficient pain relief, injection often needs to be done every one to two hours.2,6,14,31
Continuous infusion method
This method involves the attachment of the epidural catheter to an epidural infusion pump that is programmed to deliver a certain amount of pain medication continuously throughout labour. This method is often able to offer better pain relief than the intermittent method.2,6,14,31
Patient-controlled method
This method involves the attachment of the epidural catheter to a continuous epidural infusion pump set at a base rate. The woman is also given a button to push to give herself small doses of pain medication in addition to the continuous medication whenever she needs it. The pump is programmed so that a woman cannot overdose herself. This method has been found to enhance a woman’s sense of control concerning the administration of pain medication.2,6,14,31
High-concentration versus low-concentration epidural
With an epidural, a variety of different medications may be used. The amount and type of medication used can affect the degree of pain relief a woman experiences; the degree of her motor and sensory impairment; as well as the side effects she may experience.6,14,31,32
When high concentrations of anesthetic medication are used for pain relief, there is a loss of sensory and motor function from the waist downwards. This may make it difficult for a woman to feel the urge to push and as well as to move and change positions.
To decrease the motor block, a narcotic can be used in combination with a lower concentration of the anesthetic medication. This combination is becoming increasingly popular as it provides a woman with pain relief but still allows her to retain the ability feel the urge to push and potentially to walk.6,31,32
Removal of the epidural catheter
Following birth, typically a nurse or midwife removes the epidural catheter. When removing it, the woman will be asked to lean forward, the catheter will be pulled out (a black radiographic dot on its end indicates that it has been fully removed), pressure will be applied to the location to prevent bleeding, and a bandage will be applied. The woman should be instructed to tell a health care provider if she experiences any further bleeding at the site or signs of infection.14
The removal of an epidural catheter does not mean that the medication is eliminated from her body. For this reason, the first time that a woman gets up out of bed, a step-test should be performed, and she should be accompanied.
Spinal anesthesia involves the insertion of a spinal needle into a woman’s lower back to inject pain medication. A spinal needle is smaller in diameter than an epidural needle. The process of initiation of spinal anesthesia is similar to what is done to initiate an epidural. Similarly, the pain medication injected can be an anesthetic medication or a combination of an anesthetic medication and a narcotic.
For spinal anesthesia, unlike an epidural, the needle is inserted beyond the epidural space and into the subarachnoid space. The diagram below shows the placement of epidural and spinal needles. In the subarachnoid space, cerebrospinal fluid exists alongside the nerves of the spinal column. When pain medication is injected into this space, pain relief is achieved quickly. It typically takes one to two minutes for pain relief to occur which is much quicker than what occurs following the initiation of an epidural. Due to the short amount of time it takes to achieve pain relief, generally only a small, single injection of medication is needed.
Comparatively, the length of time that pain relief is provided for with spinal anesthesia tends to be limited. Spinal anesthesia typically results in the complete nerve block of the area preventing a woman from being able to move or to feel the urge to push. It is frequently used for a caesarean birth.2,14,31,32
The woman’s ability to detect being touched by ice or a pin at various points on her body helps to determine the level of the nerve block. As with an epidural, a woman’s blood pressure, heart rate, respiratory rate, and oxygen saturation are regularly checked following the initiation of spinal anesthesia. One of the major advantages of performing spinal anesthesia for a caesarean birth is that a woman is able to remain awake and avoid general anesthesia.14,32
Placement of epidural and spinal needles

A combined spinal epidural (CSE) is a type of epidural which combines features of a traditional epidural and spinal anesthesia. For a CSE, an epidural needle is first inserted into the epidural space then a spinal needle is inserted through it into the subarachnoid space. A single injection of a narcotic analgesic medication or a combination of a local anesthetic and a narcotic is injected. The spinal needle is removed, and an epidural catheter is inserted into the epidural space. This is secured to the woman’s back. A low dose of an anesthetic medication and a narcotic analgesic medication will then be infused into the epidural space through the epidural catheter either by continuous infusion or by patient-controlled infusion.2,6,14,31,32
The advantages of a CSE include:6,31,32,33,38
- Faster pain relief.
- Decreased or a nonexistent motor blockade while the initial dose is in effect.
A CSE can be referred to as a “walking epidural.” Sometimes this is a misnomer as not all women with a CSE are able to walk. If a woman wants to walk and hospital policy permits it, she should first perform a step-test to ensure that she is able to walk steadily.2,14
During the actual birth, a woman may specifically need pain medication in the area of her perineum unless she has an epidural or if the epidural is not effective. Pain medication may be needed for an assisted vaginal birth or episiotomy. Following birth, if lacerations need to be repaired, pain medication may be needed in the perineum.1,14,39
To provide pain relief to a specific area of the perineum, a physician can inject a local anesthetic medication. Epinephrine is often added to this injection to prevent excessive bleeding.14
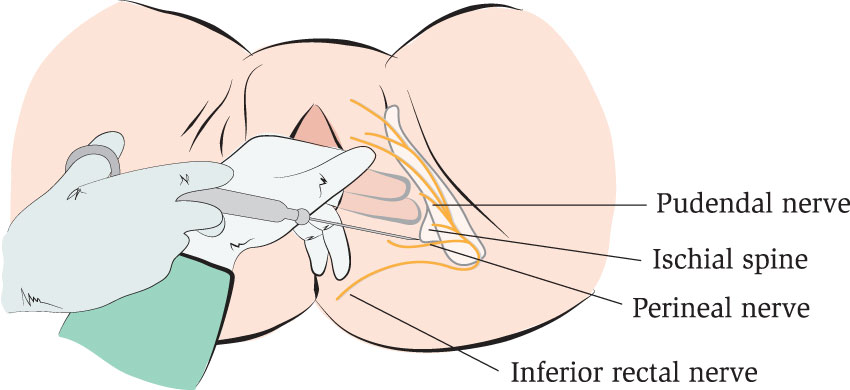
Pudendal nerve block
The pudendal nerve is the main nerve that innervates a woman’s perineum, vagina, rectum, and parts of the bladder. To provide pain relief for these areas, a technique referred to as pudendal nerve block can be done. To perform this technique, a physician injects a local anesthetic medication through a woman’s vagina and into the base of each pudendal nerve located contralaterally at the level of her ischial spines.
As the needle to perform the technique needs to first go inside a woman’s vagina, it is long. The woman should be made aware that only the tip of the needle is actually inserted. The pudendal nerve block can be used for assisted vaginal birth as well as for the repair of lacerations, tears, and episiotomies.1,2,14,31,39
Side effects associated with a pudendal nerve block are rare, but can include:1,2,14
- A decreased ability to feel the urge to push and/or bear down in the act of pushing.
- Sweating or giddiness.
- Tingling in the lower legs.
- Bleeding.
- Infection.
- Maternal anesthetic toxicity if the anesthetic is inadvertently injected into a woman’s venous system.
- Fetal anesthetic toxicity if the anesthetic is inadvertently injected the fetal head.
Coping with Adverse Reactions
One of the side effects of using narcotics for pain relief during labour is maternal, fetal, and/or newborn respiratory depression.1,6,14,40
If a woman experiences respiratory depression following the administration of a narcotic during labour, she may be given:2,14,40
- A medication called naloxone (Narcan). This is an opioid antagonist and can reverse the effects of the narcotic used. It can be given via an intramuscular injection, a subcutaneous injection, or an IV if a woman has one.
- Oxygen via a facemask or nasal prongs.
If a newborn experiences respiratory depression at the time of birth, the following will be provided:14
- Neonatal resuscitation.
- Naloxone (Narcan).
Anesthetic medication injected into the epidural space can cause blood vessels to dilate and consequently cause a woman’s blood pressure to drop. A 20 percent drop in blood pressure or a blood pressure of less than 100 mm Hg systolic can result in maternal and fetal oxygen deprivation.
If a drop in blood pressure occurs, a woman can be:14,41
- Turned on her side.
- Given a bolus of IV fluid.
- Given oxygen via a facemask or nasal prongs.
- Given an antihypotensive medication such as ephedrine or phenylephrine.
One of the risks associated with an epidural or spinal anesthesia is that the outer layer of the spinal cord, called the dura mater, can be punctured, and cerebrospinal fluid can then leak into the surrounding area. This can cause pressure to be exerted on nerves causing a woman to experience a headache. Such a headache may not present for two to three days after having the epidural and may last for days to weeks. Women who suffer a dural puncture during insertion of the epidural are usually followed by anesthesia after the birth.
If a postdural puncture headache develops, a woman can:6,14,31
- Avoid being in an upright position which often makes the headache feel worse.
- Rest in a quiet, dimly lit or dark room.
- Take oral pain medications.
- Take caffeine pills or other sources of caffeine.
- Increase her fluid intake.
The anesthesiologist may suggest doing a blood patch if the previous methods do not work to relieve the headache and if the headache is severe and interferes with the mother’s ability to care for herself and her baby. This involves the anesthesiologist taking up to 20 mL of blood from the woman’s arm and injecting it back into her lumbar epidural space. The woman should rest for one hour after this procedure is done. Sometimes more than one blood patch is needed to relieve the headache. It is effective in approximately 60 percent of cases.
Common side effects that can be associated with pain medications such as itching, nausea, and vomiting can also be treated. Antihistamines such as Benadryl can be given for itching, and antinauseants such as Gravol can be given for nausea and vomiting. If the side effects are severe, small doses of Narcan can be given as well. Typically, hospitals have a specific protocol about how such side effects are managed. In addition, as many different pain medications can cause nausea and vomiting, antinauseants such as Gravol are typically given with the pain medication to try to prevent this. An added side effect of receiving Gravol, however, is potential drowsiness.14,31
Referrals
Referrals may be warranted if:
- A woman or her support person(s) are overly anxious about coping with labour pain or medical pain-management options during labour.
- A woman or her support person(s) require more information about pain-management options during labour.
- A woman has a history of back pain, back injury, or back surgery, or is concerned that she is not a candidate for an epidural and wishes to have one during labour.
Women and/or their support person(s) who require more information and/or support leading up to labour and birth can be referred to the following sources:
- Their health care provider (obstetrician, family physician, Nurse Practitioner, or midwife) who can arrange for a referral to an anesthesiologist if necessary or wanted.
- In-person prenatal education classes, if not already enrolled.
- Their local public health unit.
Resources & Links
Professional Guidelines
- Canadian Journal of Anesthesia (CJA)
- Society of Obstetricians and Gynaecologists of Canada(SOGC)
Professional Associations
Reports/Publications
- Cochrane Database of Systematic Reviews (CDSR)
- Anim-Somuah, M., Smyth, R., & Jones, L. (2011). Epidural versus non�?epidural or no analgesia in labour. Cochrane Database of Systematic Reviews, 12(CD000331), 1-120.doi: 10.1002/14651858.CD000331.pub3
- Jones, L., Othman, M., Dowswell, T., Alfirevic, Z., Gates, S., Newburn, M., . . . Neilson, J. P. (2012). Pain management for women in labour: An overview of systematic reviews. Cochrane Database of Systematic Reviews, 3(CD009234), 1-161. doi: 10.1002/14651858.CD009234.pub2
- Novikova, N., & Cluver, C. (2012). Local anaesthetic nerve block for pain management in labour.Cochrane Database of Systematic Reviews, 4(CD009200), 1-50. doi: 10.1002/14651858.CD009200.pub2
- Othman, M., Jones, L., & Neilson, J. P. (2012). Non�?opioid drugs for pain management in labour. Cochrane Database of Systematic Review, 7(CD009223), 1-69. doi: 10.1002/14651858.CD009223.pub2
- Ullman, R., Smith, L. A., Burns, E., Mori, R., & Dowswell, T. (2010). Parenteral opioids for maternal pain management in labour. Cochrane Database of Systematic Reviews 2010, 9(CD007396), 1-217. doi: 10.1002/14651858.CD007396.pub2
- Ontario Public Health Association
- Informed Decision-Making for Labour and Birth (2017)
- Public Health Agency of Canada
- Canadian Hospitals Maternity Policies and Practices Survey(2012)
- What Mothers Say: The Canadian Maternity Experiences Survey (2009)
Websites
- Canadian Anesthesiologists’ Society (CAS)
Prenatal Education Provider Tools
- Best Start Resource Centre
- Prenatal Education Program: Module 8 - Medical Interventions & Caesearean Birth (2017)
Client Resources and Handouts
- Best Start Resource Centre (BSRC)
- Obstetric Anaesthetists’ Association (OAA)
Videos
- Bupa Health
- Injoy Health Education
- Pain Management for Childbirth, Volume 2: Analgesics and Epidurals (2011)
Apps
Appendix
References
- Jones, L., Othman, M., Dowswell, T., Alfirevic, Z., Gates, S., Newburn, M., . . . Neilson, J. P. (2012). Pain management for women in labour: An overview of systematic reviews. Cochrane Database of Systematic Reviews, 3(CD009234), 1-161. doi: 10.1002/14651858.CD009234.pub2
- McCool, W. F., Packman, J., & Zwerling, A. (2004). Obstetric anesthesia: Changes and choices. Journal of Midwifery & Women’s Health,49(6), 505-513. doi: 10.1016/S1526-9523(04)00444-1
- Ullman, R., Smith, L. A., Burns, E., Mori, R., & Dowswell, T. (2010). Parenteral opioids for maternal pain management in labour. Cochrane Database of Systematic Reviews 2010, 9(CD007396), 1-217. doi: 10.1002/14651858.CD007396.pub2
- Canadian Association of Midwives. (2010). Position statement: Midwifery care and normal birth. Montreal, QC: Author. Retrieved from http://www.canadianmidwives.org/DATA/DOCUMENT/CAM_ENG_Midwifery_Care_Normal_Birth_FINAL_Nov_2010.pdf
- Society of Obstetricians and Gynaecologists of Canada. (2008). Joint policy statement on normal childbirth. Journal of Obstetrics and Gynaecology Canada, 30(12), 1163-1165. Retrieved from http://www.jogc.com/
- Anim-Somuah, M., Smyth, R., & Jones, L. (2011). Epidural versus non�?epidural or no analgesia in labour. Cochrane Database of Systematic Reviews, 12(CD000331), 1-120. doi: 10.1002/14651858.CD000331.pub3
- Health Canada. (2000). Chapter 5: Care during labour and birth. Family-centred maternity and newborn care: National guidelines (pp.5-49). Ottawa, ON: Author.
- Lawrence, A., Lewis, L., Hofmeyr, G. J., Dowswell, T., & Styles, C. (2009). Maternal positions and mobility during first stage labour. Cochrane Database of Systematic, 2(CD003934), 1-67. doi: 10.1002/14651858.CD003934.pub2
- Lowe, N. K. (2002). The nature of labor pain. American Journal of Obstetrics and Gynecology, 186(5), S16-S24. doi: 10.1016/S0002-9378(02)70179-8
- Othman, M., Jones, L., & Neilson, J. P. (2012). Non�?opioid drugs for pain management in labour. Cochrane Database of Systematic Review, 7(CD009223), 1-69. doi: 10.1002/14651858.CD009223.pub2
- Simkin, P., & Bolding, A. (2004). Update on nonpharmacologic approaches to relieve labor pain and prevent suffering. Journal of Midwifery & Women’s Health, 49(6), 489-504. doi: 10.1016/j.jmwh.2004.07.007
- Hodnett, E. D. (2002). Pain and women’s satisfaction with the experience of childbirth: A systematic review. American Journal of Obstetrics and Gynecology,186(5), S160-S172. doi: 10.1016/S0002-9378(02)70189-0
- Hodnett, E. D., Gates, S., Hofmeyr, G. J., Sakala, C., & Weston, J. (2011). Continuous support for women during childbirth. Cochrane Database of Systematic Reviews, 2(CD003766), 1-100. doi: 10.1002/14651858.CD003766.pub3
- Perry, S. E., Hockenberry, M. J., Lowdermilk, D. L., & Wilson, D. (2013). Chapter 16: Comfort measures for labour. In C. Sams & L. Keenan-Lindsay (Eds.), Maternal child nursing care in Canada (1st ed.). (pp. 407-422). Toronto, ON: Elsevier Canada.
- Reynolds, F. (2010). The effects of maternal labour analgesia on the fetus. Best Practice & Research Clinical Obstetrics & Gynaecology, 24(3), 289-302. doi: 10.1016/j.bpobgyn.2009.11.003
- Tinti, C., Schmidt, S., & Businaro, N. (2011). Pain and emotions reported after childbirth and recalled 6 months later: The role of controllability. Journal of Psychosomatic Obstetrics & Gynecology, 32(2), 98-103. doi: 10.3109/0167482X.2011.557756
- Schuurmans, N., Senikas, V., & Lalonde, A. (2009). Healthy beginnings: Giving your baby the best start from preconception to birth (4th ed.). Etobicoke, ON: John Wiley and Sons Canada Ltd.
- Klomp, T., van Poppel, M., Jones, L., Lazet, J., Di Nisio, M., & Lagro�?Janssen, A. L. (2012). Inhaled analgesia for pain management in labour. Cochrane Database of Systematic Reviews, 9(CD009351), 1-88. doi: 10.1002/14651858.CD009351.pub2
- Public Health Agency of Canada. (2009). What mothers say: The Canadian maternity experiences survey. Ottawa, ON: Author. Retrieved from http://www.phac-aspc.gc.ca/rhs-ssg/survey-eng.php
- Better Outcomes Registry and Network (BORN) Ontario. (2013). Provincial overview of perinatal health in 2011–2012. Ottawa, ON: Author. Retrieved from http://bornontario.ca/en/resources/reports/lhin-regional-reports/
- Public Health Agency of Canada. (2012). Canadian hospitals maternity policies and practices survey. Ottawa, ON: Author. Retrieved from http://www.phac-aspc.gc.ca/rhs-ssg/chmpps-eppmhc-2012-eng.php
- Bucklin, B. A., Hawkins, J. L., Anderson, J. R., & Ullrich, F. A. (2005). Obstetric anesthesia workforce survey: Twenty-year update. Anesthesiology, 103(3), 645-653. doi: 10.1097/00000542-200509000-00030
- Hebbes, C., & Lambert, D. (2008). Non-opioid analgesic drugs. Anaesthesia & Intensive Care Medicine, 9(2), 79-83. doi: 10.1016/j.mpaic.2007.11.012
- Powell, N. D., & Riddle, D. (2014). A comparison on the effect of remifentanil patient-controlled analgesia versus fentanyl via any delivery method on maternal satisfaction and pain reduction during labor: A systematic review protocol. The JBI Database of Systematic Reviews and Implementation Reports, 12(11), 8-18. doi: 10.11124/jbisrir-2014-1549
- Evron, S., & Ezri, T. (2007). Options for systemic labor analgesia. Current Opinion in Anesthesiology, 20(3), 181-185. doi: 10.1097/ACO.0b013e328136c1d1
- Merchant, R., Chartrand, D., Dain, S., Dobson, G., Kurrek, M. M., Lagacé, A., . . . Thiessen, B. (2015). Guidelines to the practice of anesthesia. Canadian Journal of Anesthesia Volume, 62(1), 54-79. doi: 10.1007/s12630-014-0232-8
- Marwah, R., Hassan, S., Carvalho, J. C., & Balki, M. (2012). Remifentanil versus fentanyl for intravenous patient-controlled labour analgesia: An observational study. Canadian Journal of Anesthesia 59(3), 246-254. doi: 10.1007/s12630-011-9625-0
- Likis, F. E., Andrews, J. C., Collins, M. R., Lewis, R. M., Seroogy, J. J., Starr, S. A., . . . McPheeters, M. L. (2014). Nitrous oxide for the management of labor pain: A systematic review. Anesthesia & Analgesia, 118(1), 153-167. doi: 10.1213/ANE.0b013e3182a7f73c
- Rosen, M. A. (2002). Nitrous oxide for relief of labor pain: A systematic review. American Journal of Obstetrics and Gynecology, 186(5), S110-S126. doi: 10.1016/S0002-9378(02)70186-5
- Maze, M., & Fujinaga, M. (2000). Recent advances in understanding the actions and toxicity of nitrous oxide. Anaesthesia, 55(4), 311-314. doi: 10.1046/j.1365-2044.2000.01463.x
- Datta, S., Kodali, B. S., & Segal, S. (2010). Chapter 9: Relief of labor pain by regional analgesia/anesthesia. In Obstetric Anesthesia Handbook (pp. 107-149). New York, NY: Springer Science.
- Simmons, S. W., Taghizadeh, N., Dennis, A. T., Hughes, D., & Cyna, A. M. (2012). Combined spinal�?epidural versus epidural analgesia in labour. Cochrane Database of Systematic Reviews, 10(CD003401), 1-118. doi: 10.1002/14651858.CD003401.pub3
- Kuczkowski, K. M. (2007). Labor pain and its management with the combined spinal–epidural analgesia: What does an obstetrician need to know? Archives of Gynecology and Obstetrics, 275(3), 183-185. doi: 10.1007/s00404-006-0204-5
- Kukulu, K., & Demirok, H. (2008). Effects of epidural anesthesia on labor progress. Pain Management Nursing, 9(1), 10-16. doi: 10.1016/j.pmn.2007.09.003
- Mercier, F. J., & Bonnet, M. P. (2009). Tattooing and various piercing: Anaesthetic considerations. Current Opinion in Anesthesiology, 22(3), 436-441. doi: 10.1097/ACO.0b013e32832a4125
- Liston, R., Sawchuck, D., & Young, D. (2007). Fetal health surveillance: Antepartum and intrapartum consensus guideline. Journal of Obstetrics and Gynaecology Canada, 29(9 Suppl 4), S3-56. Retrieved from http://sogc.org/
- Mayberry, L. J., Strange, L. B., Suplee, P. D., & Gennaro, S. (2003). Use of upright positioning with epidural analgesia: Findings from an observational study. MCN: The American Journal of Maternal/Child Nursing, 28(3), 152-159. doi: 10.1097/00005721-200305000-00004
- Goodman, S. R., Smiley, R. M., Negron, M. A., Freedman, P. A., & Landau, R. (2009). A randomized trial of break-through pain during combined spinal-epidural versus epidural labor analgesia in parous women. Anesthesia and Analgesia, 108(1), 246-251. doi: 10.1213/ane.0b013e31818f896f
- Novikova, N., & Cluver, C. (2012). Local anaesthetic nerve block for pain management in labour. Cochrane Database of Systematic Reviews, 4(CD009200), 1-50. doi: 10.1002/14651858.CD009200.pub2
- Carvalho, B. (2008). Respiratory depression after neuraxial opioids in the obstetric setting. Anesthesia & Analgesia, 107(3), 956-961.doi: 10.1213/ane.0b013e318168b443
- Hobbs, A., & Cockerham, R. (2013). Managing hypotension during anaesthesia for caesarean section. Anaesthesia & Intensive Care Medicine, 14(7), 280-282. doi: 10.1016/j.mpaic.2013.04.002
- Dozier, A., Howard, C., Brownell, E., Wissler, R., Glantz, J., Ternullo, S., Thevenet-Morrison, K., Childs, C., & Lawrence, R. (2013) Labor Epidural Anesthesia, Obstetric Factors and Breastfeeding Cessation. Maternal and Child Health Journal, 17(4), 689-698.

